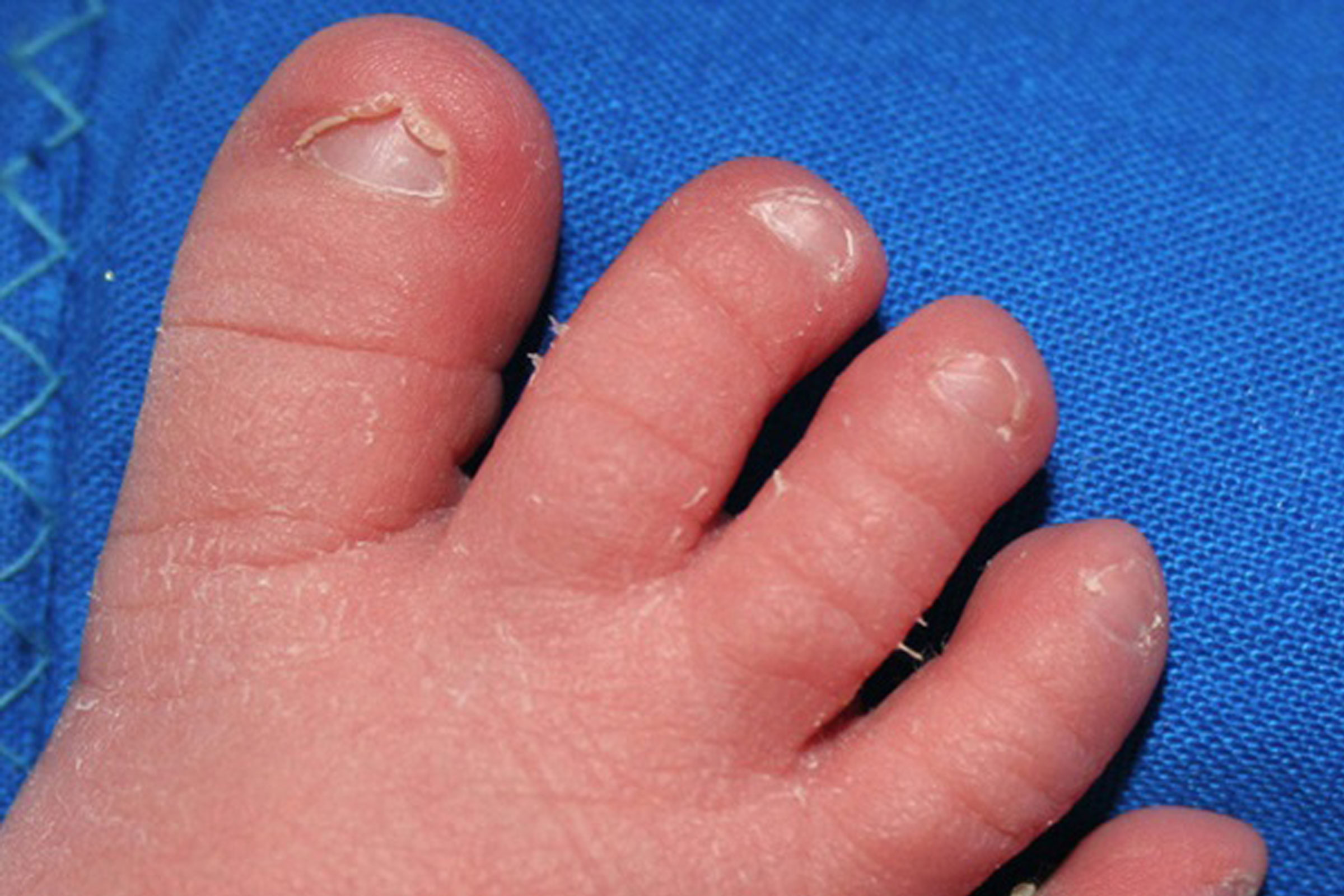
In-Grown Toe Nail
What is an In-Grown Toe Nail?
In-grown toenails are quite common, especially among teenagers. It commonly affects the big toes only and is usually the lateral aspect of the toe (i.e the side of the toe which touches the second toe). However, it can affect the other side or even both sides. In the early stages, conservative measures may be successful in treatment such as cleaning, soaking in salt baths and elevation of the nail by a small amount of cotton wool to allow it to grow out. The redness and pain of an in-grown toe nail is due to inflammation which is caused because a foreign body (the nail) digging into the skin. This can then become secondarily infected. Antibiotics can be useful in treating the infection but rarely cures the problem. In late stages, surgery may become necessary.
A wedge resection is done which excises the in-grown section of the nail and the germinal matrix, the soft tissue from which the nail grows. Recurrence of the in-grown toenail after surgery has been recorded but is rare.
Post-operative care
A dressing is placed at the time of surgery and is left untouched for 3 to 5 days. After this time, return to normal activity. Return to sports after 4 or 5 weeks.
Perianal Fistula
What is Perianal Fistula?
Perianal fistulas are very common in the first year of life and are much more common in boys than in girls. The theory here is that the small oil producing glands just on the inside of the bottom become clocked and then subsequently infected, leading to perianal abscess. Some perianal abscesses can be successfully treated by drainage with or without antibiotics however a significant number of them persist as a perianal fistula. In this situation, the perianal abscess will continue to recur until the causative tract is excised. This is done as a day stay under general anaesthetic. The tract is excised and this leaves a raw surface which is then left to heal secondarily, usually taking about 2 weeks. During this time, clean the bottom after each bowel movement as per normal.
Lung Abnormalities
What are Lung abnormalities?
Lung abnormalities can be picked up by antenatal ultrasounds.
The more common lesions include:
Bronchogenic cyst
A bronchogenic cyst is a fluid filled cyst usually made up of abnormally sited respiratory tissue. These lesions usually occur near the major airways leading to the lungs, but may occur more peripherally in the lung. They carry risk in that they can become infected and tend to enlarge over time, possibly causing a compression of the major airways going into the lung. Recommended treatment is surgical excision that we usually perform using thoracoscopic (keyhole) surgery.
Bronchopulmonary Sequestration (BPS)
A bronchopulmonary sequestration is an abnormally developed piece of lung tissue that obtains its blood supply from the systemic rather than pulmonary blood flow. The lesion may be attached or separate from the lung. A BPS may also containelements of a CPAM (hybrid lesion). The management of this lesion would depend on its size and the size of the abnormal blood supply feeding it. They are often managed in a similar way to a CPAM.
Duplication Cyst
This represents a cyst that arises from an attempt to replicate part of the intestinal tract, in the chest this is usually the oesophagus. It is usually attached to the oesophagus and can cause symptoms by obstructing the oesophagus, becoming infected or bleeding. As such we recommend removal which we usually perform using thoracoscopic (keyhole) surgery.
Congenital Pulmonary Airway malformation (CPAM)
This is the most common cause of cystic lung abnormality in children. The true incidence is not known but is thought to range between 1:4000- 1:8000 births. These may present antenatally (during your pregnancy) on routine ultrasound screening, following birth or at any time during childhood. The range of presentations may be related to the size of the CPAM or complications arising in the CPAM. Most often however, children will have very few to no symptoms. Complications that may arise in the CPAM are secondary to the compression of the normal lung or heart by the lesion, infection (thought to be 5-10%) and rupture of the lesion causing a pneumothorax (leakage of air around the lung). Most of these complications are uncommon. There has been a reported association between CPAM and malignancy in later life. This link however is tenuous and unproven. Treatment depends on the size, and consistency of the CPAM as well as the likelihood for complications.
Congenital Lobar/ Segmental Emphysema
This represents a part of the lung with abnormally dilated airspaces, which may in some instances cause compression of the adjacent normal lung. These lesions may be asymptomatic at birth but as they enlarge, they become symptomatic in the first few weeks to months. Only lesions that produce symptoms require surgery.
Treatment
Antenatal Management
When a lung lesion has been diagnosed we would recommend consultation with a paediatric surgeon experienced in the management of paediatric thoracic surgery. We would then explain the natural history throughout the pregnancy and provide a plan of management once your baby is born.
Post-natal Management
Once babies with a lung lesion are born they are observed to ensure they do not have breathing difficulties and furthermore are able to feed well. A chest x-ray and review is recommended at birth. If your child is well they can then be discharged with a follow up at 1 month to ensure they continue to thrive and have not developed symptoms over time. Thereafter, a consultation at 3 months is recommended if they remain well.
CT scan is further recommended after 1 years of age to provide detail on the size and location of the lesion. The CT scan will need to be performed under a general anaesthetic and this is best performed at a children’s hospital. The next consultation will review the CT scan and detail the size, morphology, and likelihood of developing problems. This will permit us to make a recommendation on either a long term follow up or surgical intervention. This plan is developed in a consultation with the parents, ensuring they understand the benefits and risks with each approach.
Surgery
The removal of a lung lesion is undertaken on lesions that cause symptoms, or that are likely to cause problems with the development of the normal lung or complications later in life. Almost all of our procedures are undertaken via thoracoscopic (keyhole surgery). If the surgery is not possible thoracoscopically then the operation is performed through a small curved incision around the shoulder blade, working between the muscles to minimize post-operative pain. The duration of stay ranges from 3 to 7 days depending on the approach required. Usually a small chest tube is left post operative for 2 to 3 days.
Hydrocoele
What is a Hydrocoele?
A hydrocoele is a collection of fluid around the testis. The testis first develops near the kidney when the baby boy is inside the mother’s womb. For the testis to drop down into the scrotum there needs to be a passage through the groin area. Normally this closes off around the time of birth.
If the passage stays open, fluid can pass from the tummy cavity and surround the testis. Even when there is a lot of fluid, it does not harm the testis in any way.
As the communication may close without an operation, we generally wait until the boy is about 18 months of age before recommending surgery. If the hydrocoele does not resolve by this age, an operation is advised as the fluidcollection may become uncomfortable for the boy as he becomes older.
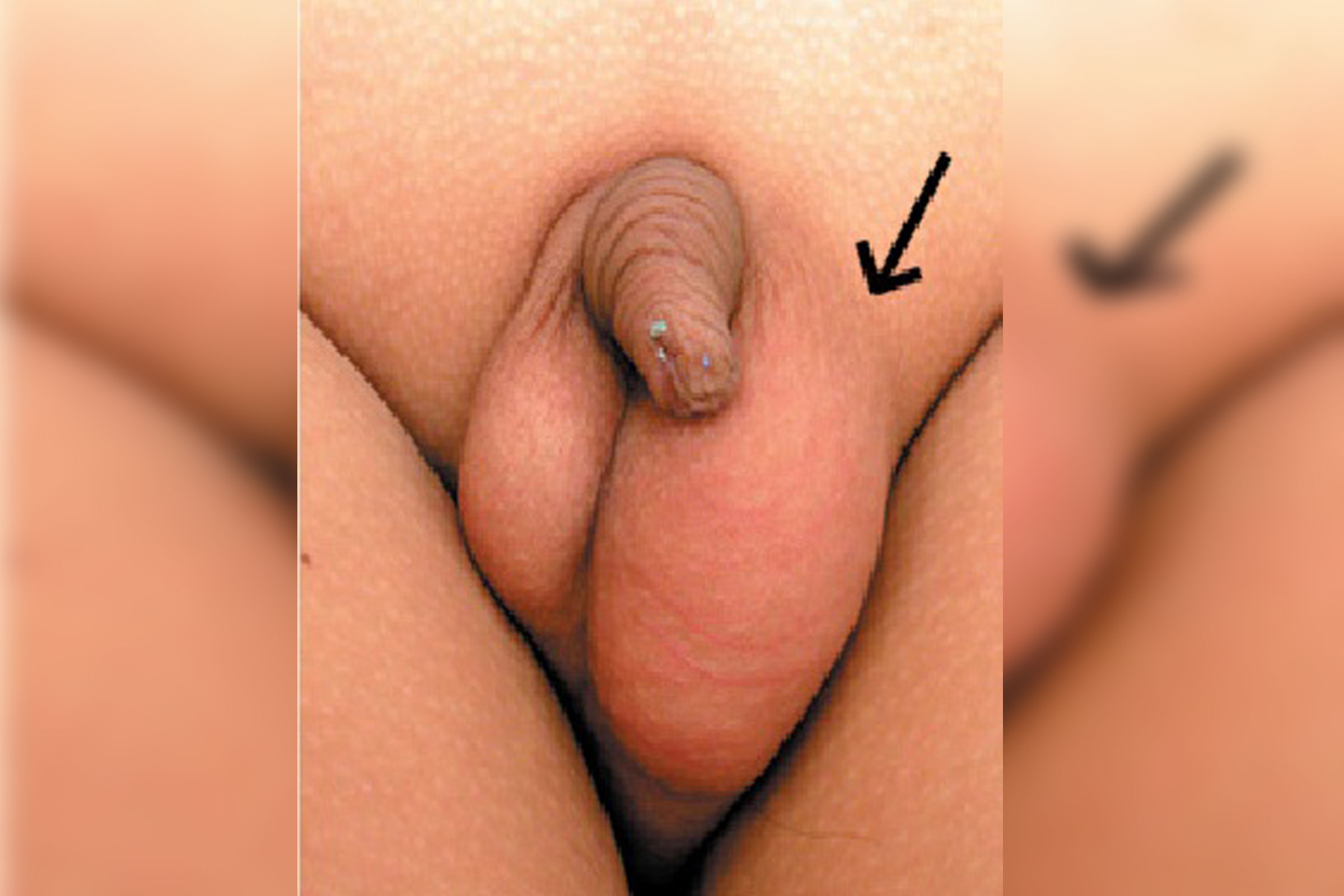
General description
The aim of the procedure is removal of the communication between the tummy cavity and the testis. The operation is performed as a daycase under general anaesthesia. Generally the operation takes about 40 minutes.
Preparations
Your child will need to fast for solids and liquids generally for about 6 hours before the start of the procedure. In breast-fed babies or infants this time may be reduced after consultation with the anaesthetist. Please ring the Day Surgery Unit the working day before surgery to confirm these times. It is often helpful to bring your child’s favorite toy with you on the day.
Anaesthesia
You and your child will meet the anaesthetist on the morning of the procedure. After talking to you and briefly examining your child, they will take you through to the operating theatre. One parent is welcome to accompany your child until they are asleep. The anaesthetist puts your child to sleep via a face mask (with children 5 years and over there is the option of either a face mask or a needle with numbing cream).You will then be shown the waiting room where there is tea, coffee or water available to drink. Once your child is asleep, the anaesthetist will insert a ‘drip’ to allow fluids to be given directly into a vein. Usually this is located in the hand or arm, but occasionally may need to be sited in the leg or scalp.
Procedure
The groin area is cleaned with an antiseptic solution. A local anaesthetic block is injected into the area so that the site of the operation is numb after the operation. This block usually lasts for about 4 to 6 hours. A cut is made in the groin on the side of the hydrocoele. Once the communication between the tummy cavity and the testis has been found,two important tubes need to be peeled off it: the blood vessel to the testis and the sperm tube. The communication can then be tied off and fluid removed from around the testis. The wound is then closed with dissolving stitches which are buried under the skin. A clear, water-resistant dressing is then placed over the wound.
Initial recovery
After the operation has finished, your child will be taken to the recovery area. Once awake, you will be called into the recovery ward. Often children appear distressed and a little confused initially – there may be several reasons for this including residual effects of the anaesthetic, hunger, and some discomfort. Generally they will settle quite quickly, especially if offered a drink or feed. The recovery and ward staff are also able to give pain relief medication once your child is awake, and this is sometimes required.The nursing staff will check the wound and make sure you are happy before you go home. Usually this will be about 2 hours after the surgery.
As a result of the local anaesthetic nerve block, your child may complain of a numb sensation in the groin and in some cases some weakness in the leg on the side of the surgery. This is temporary and will generally settle within a day or so of the operation.
Post-operative course
There may be a small amount of blood that oozes from the edges of the dressing, enough to lightly stain a nappy or pair of underpants. Paracetamol (‘Panadol’) should be given on the afternoon and evening of surgery, and in the morning of the following day. Older children may require a stronger medication such as ‘Painstop Day-time’ or ‘Painstop Nighttime’ if over one year of age. After that time, assess your child’s pain to see if further doses are required. Follow the manufacturer’s dose instruction but never give more than 4 doses in a 24-hour period and never both at the same time. Your child should not be bathed on the first night, but nappies can be changed as required and a ‘wetwipe’ of similar cloth used. Showers are safe from the next day onwards. There may be a small amount of blood that oozes from the wound under the dressing in the first 24 hours. Generally the dressing does not need to be changed, but if you are concerned please discuss with your local doctor or myself. It is quite normal for the scrotum and testis to swell after the operation and there may also be some bruising. It is not the hydrocoele returning but the body’s normal response to the operation and settles within the first few weeks. You should remove the dressing completely after a long bath on the fifth day after the operation. No further dressings are then required. Your child will have stitches underneath the skin which will dissolve.
Your child can begin eating when he gets home. Start with clear liquids (apple juice, iceblocks) and add solid food slowly and in small amounts. Your child may vomit from the anaesthesia on the day of surgery. This should stop by the morning after surgery.
Return to activity
Your child may return to day care or school when comfortable, usually within 3-5 days. He should not participate in sports or swimming for 3 weeks after the surgery and should not ride straddle toys (bikes, walkers) for 2 full weeks after surgery. You should continue to use your car seat.
Call our office if:
- You see any signs of infection: redness along the incision site, increased swelling, foul smelling discharge from incision
- Your child’s pain gets worse or is not relieved by painkillers
- There is bleeding (small ooze of blood in the first day or two is normal)
- Your child has a high temperature
- Vomiting continues on the day after surgery
- You have any questions or concerns
Follow-up
Normally I see you and your child about 3 to 6 weeks following surgery. This is both to ensure that the wound has healed and that you and your son are satisfied with the results of the operation. For patients from rural areas, this review may be deferred to your own general practitioner if you prefer. Please ring soon after the operation to book the post operative appointment to arrange a convenient time.
Problems & further surgery
Generally this procedure is straightforward, but there is a 5% chance that the hydrocoele may not resolve completely following the surgery. In the majority of these cases the fluid is re-absorbed by the body over the next 6 to 12 months. Rarely, a further operation will be required. During the operation there is a very small risk (less than 1%) of damage to the blood vessels to the testis and the sperm tube. This risk is minimised by the use of magnification during the procedure and usually can be both detected and repaired at the time of operation should this occur. As with any surgical procedure, there is always a 2-3% risk of a wound infection or bleeding after surgery.

